Pulmonary embolus (PE)
Information for patients
What is a pulmonary embolus?
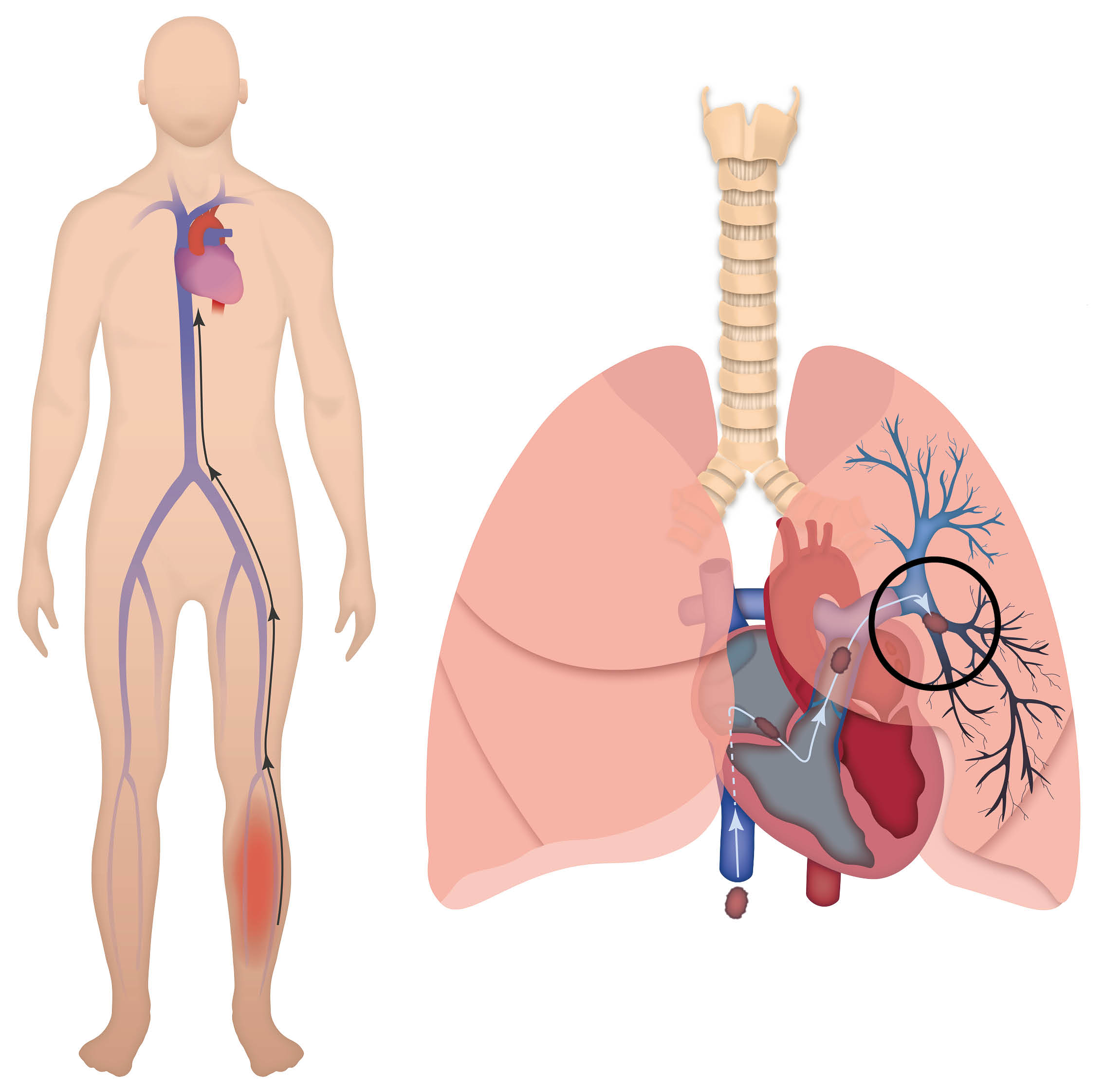
A pulmonary embolus (PE) is a blood clot lodged in one or more of the pulmonary arteries in the lung.
A PE usually originates from a deep vein thrombosis (DVT). A DVT is a blood clot in the deep veins, usually in the leg.
What are the symptoms of a PE?
Symptoms will vary depending on the size and position of the blood clot. Not everybody will have all these symptoms.
Shortness of breath, either at rest or on exertion. This is due to the blood clot restricting the arterial blood flow through the lungs. In some cases, you may need oxygen to help with this.
An increased heart rate. This is due to the heart having to work harder to make sure enough oxygen is moved around the body.
Chest pain. This may be constant or only when breathing deeply. This is due to inflammation in the lungs or the lining of the lungs.
Coughing up blood or blood stained sputum. This is rare and will stop. Rare means it happens to between 1 in 1000 and 1 in 10,000 people.
What tests will I have in hospital?
Vital signs monitoring. We will check your oxygen level, heart rate, blood pressure, respiratory rate, and temperature regularly. This helps to see how hard your heart is working and how effective your breathing is. It may also help to rule out infection.
We will take blood tests to make sure your body is able to cope with the medication needed. We may also measure your inflammatory markers to make sure there is no infection.
An ECG (electrocardiogram) shows the electrical activity of your heart. Whilst often not affecting the heart directly, an ECG can sometimes suggest a PE.
A chest x-ray is not able to diagnose a PE, but it can rule out other possible conditions, such as a chest infection.
A VQ (Ventilation and Perfusion) scan looks at the air and blood flow in your lungs. A CTPA (Computed Tomographic Pulmonary Angiography) scan looks at the arteries in your lungs. We may use either scan to diagnose a PE.
Each test involves us inserting a cannula into a vein in your arm, and an injection of ‘dye’. This allows us to see if you have a PE. Sometimes the ‘dye’ used may give the feeling that you are urinating when you are not. This usually stops quickly.
After a clinical assessment you may need other investigations. Not all tests will need to be done urgently.
Once diagnosed, what is the treatment of a PE?
Your body will naturally break down the blood clot. To do this safely you will need to take anticoagulant medication. Anticoagulant medication will thin your blood to prevent:
the blood clot from getting bigger or moving; or
new clots from forming.
We may give you anticoagulant medication as warfarin tablets, heparin injections, a combination of the two, or a newer oral anticoagulant class called direct acting anticoagulants (DOAC).
Warfarin tablets come in three different colours and doses:
1mg: brown tablets
3mg: blue tablets
5mg: pink tablets
When taking warfarin, you will have regular blood tests to monitor your INR (International Normalised Ratio). This is a measure of how long it takes for your blood to clot.
The dose of warfarin we prescribe will differ according to your INR. Your specialist will tell you what to take and when, depending on the results of your blood test.
Heparin injections are given according to your weight and kidney function. Heparin is usually given once a day (occasionally twice daily) into the skin in your abdomen (tummy). A nurse may show you how to do this yourself, or a nurse may do it for you.
Rivaroxaban is an oral anticoagulant. If taken from when we diagnose the blood clot, you need to take this twice a day for 3 weeks and then once each day after that. After the first 3 week period, the dose usually does not change. There is no need for blood tests to check its effect.
We will check your kidney and liver blood tests before and every 3 to 6 months during treatment with this drug. This is how your body processes the drug.
Apixaban is an oral anticoagulant. If taken from when we diagnose the blood clot, you take a higher loading dose for 1 week, and continue on a fixed dose twice daily after that. After the first 1 week loading period, the dose usually does not change. There is no need for blood tests to check its effect.
We will check your kidney and liver blood tests before and every 3 to 6 months during treatment with this drug. This is how your body processes the drug.
Other oral anticoagulants are dabigatran, edoxaban, and acenocoumarol. We will only advise you to use these if they have advantages for you compared to the ones mentioned above. You should only be on one anticoagulant.
What are the side effects of anticoagulants?
All anticoagulants increase your risk of bleeding, as they thin your blood. Be extra careful when cutting your nails, shaving, or using sharp implements. If you do have any bleeding, apply extra pressure on the affected area and get medical help if it does not stop.
Some people complain of feeling cold when taking anticoagulants.
Heparin can cause your platelets (a clotting component in the blood) to drop in the first few weeks of taking it. We will test your blood regularly when you first start taking heparin to see if this happens.
There are some medications (such as aspirin), which you should often not take with anticoagulants. Some herbal medications and food also interact with certain anticoagulants. Your specialist will advise you.
If your doctor or nurse prescribe you any new medication, tell them that you are taking warfarin. They will need to check for any possible interactions.
What will happen if I do not want to take anticoagulants?
You are strongly advised to take the anticoagulants. If you do not take them the blood clot could get larger, causing further damage to your lung. If this happens it can further restrict your breathing. The clot could also break up and block further arteries.
If untreated, a PE can be fatal. Most people who have a PE and take anticoagulants recover without complications.
Do I need to stay in hospital?
Not all patients need to stay in hospital. It will depend on the size and position of your PE, and how it affects you.
If you have a fast heart rate, fast breathing, or are in severe pain, you may need to stay in hospital for a few days. This may be between 1 and 7 days.
If you are relatively well with your PE, we may treat you as an outpatient on the Ambulatory Care Pathway. If you want more details about the pathway, please speak to a member of staff.
How long will I need to take anticoagulants?
You will need anticoagulant medication for at least 3 months.
If you are taking warfarin
Once your INR becomes ‘therapeutic’ (has reached the desired level), we will refer you to the Anticoagulant Clinic as an outpatient. This is usually between 5 and 7 days after starting warfarin. The clinic staff will continue to check your INR and warfarin. Once your INR is ‘stable’ (remains at an acceptable level), we will refer you to an Anticoagulant Clinic closer to your home.
If you are on rivaroxaban, apixaban, or heparin injections
We will refer you to the Anticoagulant Clinic early on in your treatment. The specialist staff at the clinic will tell you how long they will treat you for. They will arrange follow-up appointments as needed.
What can I do to help my recovery?
Listen to your body. If you do anything that makes you feel breathless or increases your pain, stop.
Do not drive, go on long walks, or exercise (such as gardening or going to the gym), until you have spoken to your specialist. You will be able to return to your normal lifestyle in time.
Until the PE starts to improve, you may feel some discomfort. Take the painkillers we have prescribed for you. Avoid over-the-counter medicine, unless you have discussed this with your specialist.
When sitting, keep your legs elevated (raised), ideally above the level of your hips, unless told otherwise by your specialist. This will help with your blood flow and reduces leg swelling.
Look after yourself. Eat a healthy diet and drink plenty of fluid. To begin with you may not be able to move around as normal, due to pain and breathlessness. This will increase your risk of getting constipation.
When should I call for help?
If your symptoms get worse (chest pain increases or your breathlessness worsens) get checked at your nearest hospital. If severe, call 999.
If you have any bleeding which you cannot stop, go to your nearest hospital. If you cough up blood, contact your specialist, your GP, or call 111 for advice.
Ask 3 Questions
There may be choices to make about your healthcare. Before making any decisions, make sure you get the answers to these three questions:
What are my choices?
What is good and bad about each choice?
How do I get support to help me make a decision that is right for me?
Your healthcare team needs you to tell them what is important to you. It’s all about shared decision making.
What do you think of this leaflet?
We welcome feedback, whether positive or negative, as it helps us to improve our care and services.
If you would like to give us feedback about this leaflet, please fill in our short online survey. Either scan the QR code below, or use the web link. We do not record your personal information, unless you provide contact details and would like to talk to us some more.
If you would rather talk to someone instead of filling in a survey, please call the Patient Voice Team.
Patient Voice Team
Telephone: 01227 868605
Email