Jaw joint problems
Information for patients from the Oral and Maxillofacial Department
This leaflet is for patients who have been referred to the Oral and Maxillofacial Department with a jaw joint problem. This leaflet explains the following.
What the jaw joint is.
What the causes and symptoms of a jaw joint problem are.
What treatments are available.
What happens if these treatments do not work.
We hope this leaflet answers some of the questions you may have. If you have any further questions or concerns, please speak to a member of your healthcare team.
Where is the jaw joint?
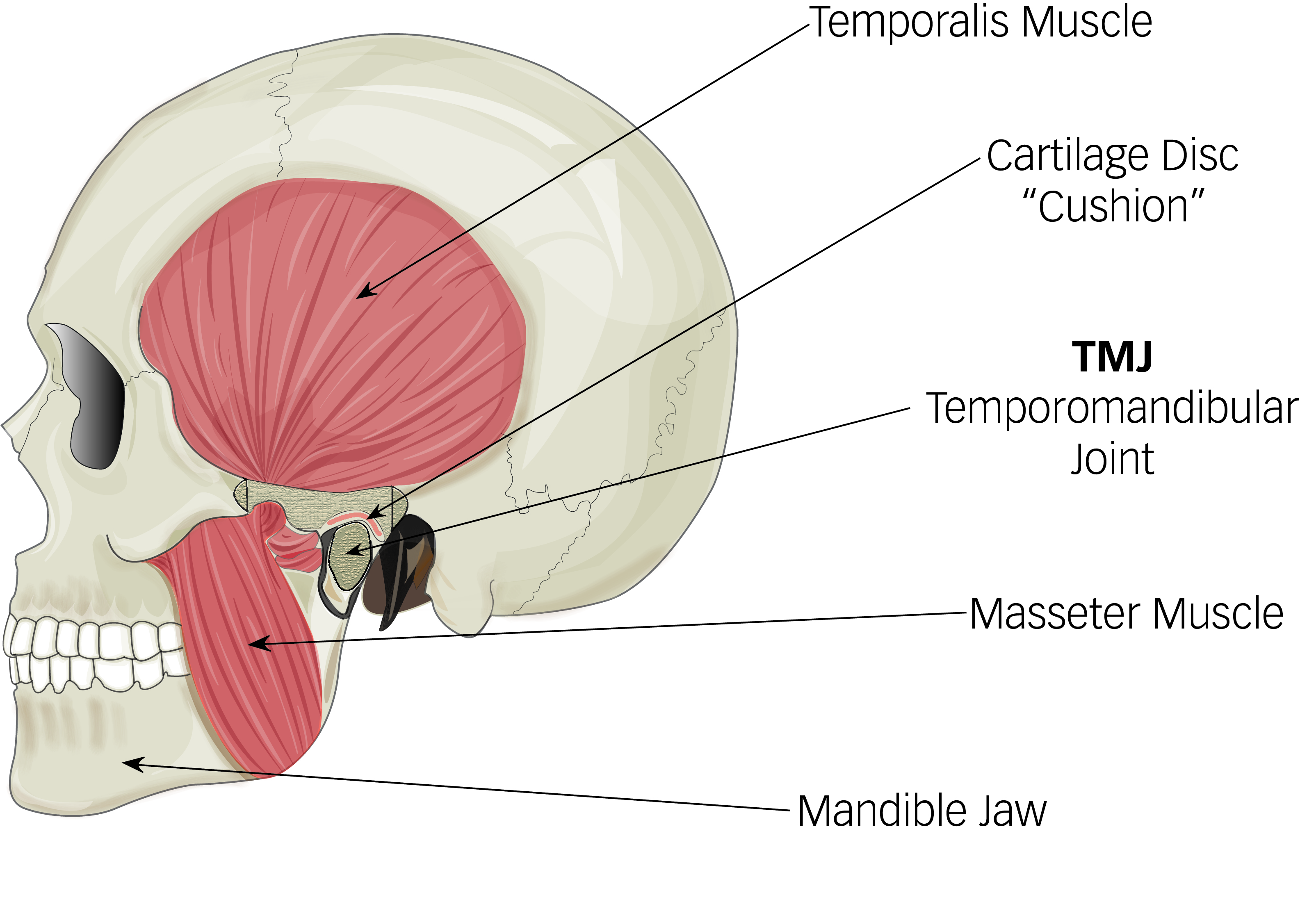
The temporomandibular (jaw) joint is found in front of your ear, where your skull and lower jaw (mandible) meet. The joint allows your lower jaw to move and function.
The joint is made up of two bones separated by a disc of cartilage. Ligaments and muscles surround the joint.
What are the symptoms of jaw joint problems?
Problems with the jaw joint are very common, but usually only last a few months before getting better.
In some cases only the muscles are affected (myofascial pain dysfunction). In other cases the cartilages and ligaments may also be faulty. This can lead to conditions such as internal derangement of the temporomandibular joint.
The most common symptoms are:
Joint noise such as clicking, cracking, crunching, grating, or popping.
Pain, usually a dull ache in and around your ear. The pain may radiate (move forwards) along your cheekbone or downwards into your neck.
Headache.
Not being able to open your mouth fully.
Chewing can make most jaw joint problems worse, and stress can aggravate them.
What causes jaw joint problems?
The tightening-up of muscles in and around your jaw joint can cause pain.
Joint noise happens if the disc of cartilage moves out of its normal position, between the bones of your jaw joint. Often the cartilage slips forwards and makes a noise when it returns to its normal position. The noise sounds louder to some patients than others, because the joint is just in front of the ear.
The ligaments and muscles surrounding the joint can go into spasm. If this happens it can lead to pain and problems with opening your mouth fully.
Why have I got jaw joint problems?
The cartilage in your jaw slips forward due to over-use of the muscles surrounding your jaw. The over-use commonly causes tightening of your muscles. This may happen as a result of chewing habits, such as grinding or clenching your teeth when under stress or at night.
Nail biting or holding things between your teeth can also cause jaw joint problems.
Certain medications are known to contribute to clenching and grinding. If you take any of the following medications, please speak to your GP about changing them.
Citalopram (Celexa)
Escitalopram (Lexapro)
Fluoxetine (Prozac)
Fluvoxamine (Luvox)
Paroxetine (Paxil)
Sertraline (Zoloft)
Vilazodone (Viibryd)
Levomilnacipran (Fetzima)
Milnacipran (Savella)
Venlafaxine (Effexor)
Medication used to treat ADHD and Parkinson’s disease, and anti-psychotic medications can also cause clenching and grinding. If you take medication for any of these conditions and clench or grind your teeth, please speak with your GP about possibly changing your medication.
Less often missing back teeth, an uneven bite, or an injury to your jaw can lead to the problem.
Often no obvious cause is found.
Are my problems anything to worry about?
Jaw joint problems are not usually serious. They do not lead onto other problems, such as arthritis of the jaw joint. They can be a nuisance though. Fortunately, jaw joint problems usually respond to simple treatments.
What are the treatments?
Treatment varies, depending on whether you are suffering from:
myofascial pain dysfunction
internal derangement of the temporomandibular joint; or
a combination of both.
Treatment is mainly aimed at trying to reduce the workload of your jaw muscles. This will allow the disc of cartilage to return to a normal position in your joint.
A soft diet that needs little chewing, allows over-worked muscles to rest.
Painkillers / anti-inflammatory medication (such as ibuprofen) are good. They can be taken as either tablets or applied as a gel to the outside of your joint.
Heat, for example warm water in a hot water bottle, wrapped in a towel placed on the side of your face. Do not use boiling water.
Identifying and stopping any habits, such as clenching or grinding your teeth. Remember, these may be subconscious (you may not be aware of them).
Resting the joint as much as possible. Try to avoid yawning.
A clear plastic splint (soft bite raising appliance) that fits over your teeth. The splint is worn mainly at night, and helps support the joint and surrounding muscles. For more information, ask a member of staff for the Caring for your soft bite raising appliance (BRA) advice sheet.
Physiotherapy (see below).
Replacing missing teeth to balance your bite. If this is appropriate, your doctor will have discussed this with you.
Relaxation therapy and learning ways to control tensions and stress.
Your doctor will have discussed jaw joint exercises with you. Please follow these carefully.
You and your doctor will discuss which of the above treatment options is best for you.
[Web site last accessed 18 December 2025]
Physiotherapy: TMJ (temporomandibular joint) exercises
Your clinician will go through the following exercises with you. Please perform these exercises each day until your symptoms improve.
Your condition is chronic (long-term). You will have flare-ups at different times of your life.
If you experience pain while doing these exercises, please take over-the-counter pain killers (such as paracetamol). Follow the instructions on the packaging. If you need further help with your pain, please speak to your GP.
Wearing your splint will help relieve pressure on your teeth. If you clench or grind your teeth, the splint will not cure this. If you need more splints, these are made by your local dentist.

Posture
Sit on a straight backed chair. Let your back relax and sit slightly rounded.
Sit tall, lifting your chest. Use your back muscles to straighten your back, this may arch it (not too much).
To support and maintain this position, use a rolled-up towel behind your low back.
Sitting tall places your head back on top of the shoulders. It also places your jaw in a more middle position, rather than your lower jaw resting forward in the joint.
Relaxed jaw position
Have your lips together and your teeth slightly apart.
Place your tongue as flat as you can on the roof of the mouth.
Breathe through your nose rather than your mouth.
Do this exercise regularly to relax your jaw. Set an alarm to remind you to improve your jaw position.
Improving control exercise
Repeat this exercise approximately 10 times. Try less or more times, depending on how your jaw feels.
To improve control, you can place your tongue on the roof of your mouth during this exercise.
To progress, remove your finger from your chin. Start by opening your mouth slightly, and progress to fully opening your mouth.
-
.jpg) Place one finger on your jaw joint, to make sure there is no clicking.
Place one finger on your jaw joint, to make sure there is no clicking. -
.jpg) Place another finger on your chin. Add pressure towards your chin, to avoid pushing your lower jaw forward too much.
Place another finger on your chin. Add pressure towards your chin, to avoid pushing your lower jaw forward too much. -
.jpg) Slowly open and close your mouth. Aim for the movement to be in a straight line and smooth.
Slowly open and close your mouth. Aim for the movement to be in a straight line and smooth.
Isometric stabilising exercises
Do not do the following exercises if you have a clicking jaw, or you have a closed or open locked jaw.
-
.jpg) Start in the resting jaw position.
Start in the resting jaw position. -
.jpg) Place your thumb under your chin. Try to open your mouth, but stop yourself by using your thumb. Hold for 10 seconds. Repeat until you feel tired. Repeat the exercise with your mouth open slightly.
Place your thumb under your chin. Try to open your mouth, but stop yourself by using your thumb. Hold for 10 seconds. Repeat until you feel tired. Repeat the exercise with your mouth open slightly. -
.jpg) Place your thumb on the right side of your jaw. Try to push your jaw to the left, but stop yourself by using your thumb. Hold for 10 seconds. Repeat until you feel tired. Repeat the exercise in the opposite direction.
Place your thumb on the right side of your jaw. Try to push your jaw to the left, but stop yourself by using your thumb. Hold for 10 seconds. Repeat until you feel tired. Repeat the exercise in the opposite direction.
Massage
Facial massage helps to relax your facial muscles, and keep the muscles around your jaw and forehead flexible.
Use a gentle moisturiser or oil.
Massage your jaw / cheek area, temple region, and forehead.
Massage in slow, smooth, circular movements, for 2 to 5 minutes.
Massage and stretches for inside the cheek
Place your thumb or a spoon on the inside your mouth, and your index finger on the outside (a pincher grip).
Push your thumb / spoon outwards into your cheek, in scooping movement. Push out in the direction of a clock, for example towards 1, 2, 3, 4, 5 o'clock. Hold each movement for 5 seconds.
Repeat 5 to 10 times slowly.
-
.jpg) Using the thumb and index finger
Using the thumb and index finger -
.jpg) Using a spoon and index finger
Using a spoon and index finger
What happens if these treatments don't work?
If the treatments listed above do not work, you can try therapeutic interventions. These are only carried out in a small number of cases. Therapeutic interventions involve:
the manipulation of your joint whilst you are asleep; or
more rarely, surgery carried out with a mini telescope.
In extreme cases we may need to surgically open your joint and operate on the bones, cartilages, and ligaments.
Are jaw joint problems anything to worry about?
It is important to realise that jaw joint problems, although a nuisance, are not sinister. They usually respond to simple treatment over time. Patients can manage most of these treatments themselves.
Occasionally, jaw joint problems may return after several years. It is very rare for jaw joint problems to progress to arthritis.
What do you think of this leaflet?
We welcome feedback, whether positive or negative, as it helps us to improve our care and services.
If you would like to give us feedback about this leaflet, please fill in our short online survey. Either scan the QR code below, or use the web link. We do not record your personal information, unless you provide contact details and would like to talk to us some more.
If you would rather talk to someone instead of filling in a survey, please call the Patient Voice Team.
Patient Voice Team
Telephone: 01227 868605
Email