Dupuytren's disease: needle aponeurotomy procedure
Information for patients from the Orthopaedic Hand Service
You have been referred for a procedure to correct Dupuytren's contracture. This will be done using a needle aponeurotomy technique, also known as fasciotomy. This leaflet explains the following.
What Dupuytren's disease and Dupuytren's contracture are.
What a needle aponeurotomy procedure is.
What the benefits and risks are to having this procedure.
How to care for your hand after surgery.
When you can return to your normal activities.
We hope this leaflet answers some of the questions you may have. If you have any questions or concerns, please speak to a member of the Orthopaedic Hand Service.
What is Dupuytren’s disease and Dupuytren's contracture?
Dupuytren’s disease is a condition that affects the hands and fingers.
Dupuytren’s disease happens when a small lump of tissue develops in the connective tissue of the palm. The lump usually develops where your ring and small fingers meet.
Over time the lump can develop into a fibrous rope like cord, connecting your palm to one or more of your fingers. As this happens your finger pulls down, making it difficult to fully straighten your finger. This condition is known as a Dupuytren’s contracture.
For more information, please read the Dupuytren's disease leaflet.
What is a needle aponeurotomy procedure?
During the procedure, your surgeon will insert a sharp blade or a very fine needle into the fibrous bands in the palm of your hand / fingers. They will use the blade or needle to divide the cord under your skin. By doing this they will release the tightness in your hand, that is forcing your finger to bend.
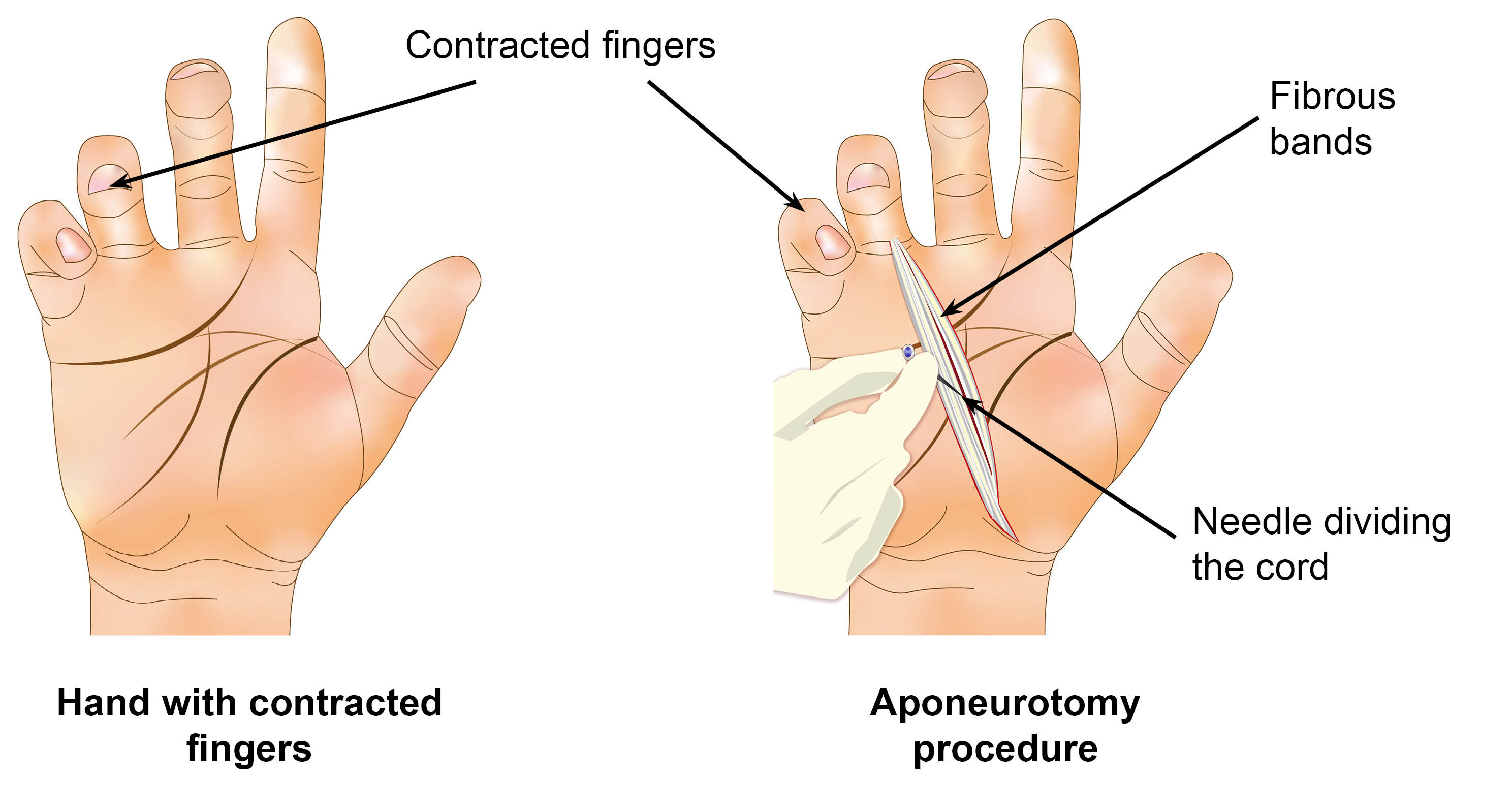
Needle aponeurotomy can be suitable:
for older patients who are unsuitable for surgery; or
if the contracture is only affecting the knuckle joint.
What are the benefits to having this procedure?
Your fingers are less deformed.
You recover more quickly compared to more extensive surgery.
It has a low risk of complications. Around 1 in every 100 patients will have a complication.
What are the risks and possible complications from this procedure?
As with any surgery, complications can occur. However, with Dupuytren’s contracture they tend to be mild, if they happen at all. Complications can include the following.
Incomplete correction. It may not be possible to fully straighten the finger. Particularly if the finger has been bent for many years.
Delayed wound healing or infection. A small number of patients may develop an infection, and need antibiotics or a wash out procedure (more common in patients with diabetes).
Compared to non-smokers, smokers are more likely to have complications in tissue healing and infections after injuries or surgery. For free friendly support and medication to help you stop smoking, contact One You Kent.
One You Kent
Telephone: 03001 231 220
Email
Nerve injury. The contracted tissue is wrapped around the small nerves in the finger. Five to 10 in every 100 patients may have some permanent or temporary loss of feeling along their finger.
Collection of blood or blood clots in the hand tissues (haematoma). This may need a second surgical procedure to remove the blood clot.
Recurrence. The rate of recurrence for Dupuytren’s contracture is very high. As many as 6 in every 10 people who have this procedure will have Dupuytren’s contracture again within 3 to 5 years. We select patients carefully to get the best outcome.
Complex regional pain syndrome (CRPS) is a rare condition. It can cause severe pain, swelling, and stiffness in the hand. This can take several months to improve or may even continue.
Please remember that most patients have an uncomplicated routine procedure. They are very satisfied with their recovery and outcome.
What happens if I choose not to have surgery?
If you choose not to have surgery, there is a possibility the contracture may continue to develop. It could pull your finger(s) closer to your palm. This may make it harder to use your hand for daily activities. However, in some cases the contracture does not change.
If your finger is very contracted, the surgical release becomes more challenging. You may not get a completely straight finger if you choose to have surgery at a later date.
Will I have to stay in hospital overnight?
No, this is a day case procedure. You will be in the hospital for a few hours only, and can then go home.
Will I have an anaesthetic?
Yes. We will give you a local anaesthetic before your procedure. The anaesthetic will numb your hand, but you will be awake the whole time.
How do I care for my hand after my procedure?
After your procedure, we will cover your small wound with a plaster. We will put a bandage over the plaster. You must keep your dressings dry. After the first 2 days remove the bandage. Leave the plaster in place for a further 7 to 10 days.
It is important to keep your hand elevated (raised), above the level of your heart, as much as possible. Please do this for the first 1 to 2 days after your procedure, to reduce any swelling.
You may have a dissolvable stitch, which will fall out around 10 to 14 days after your procedure. At that time, when your wound is completely dry and scabbed over, you may wash your hand under a running tap.
What should I do if I feel pain at home?
You will feel a little discomfort and have some bruising after your procedure; this is normal. Take simple painkillers (such as paracetamol) if needed, and you are able to take this type of medication.
If your pain becomes much worse when you arrive home and you start to feel unwell, contact your GP for advice and pain relief. If this is outside GP hours, go to your nearest Urgent Treatment Centre or Emergency Department. They may need to check your wound.
How do I care for my scar?
Once a scar has formed, it may become sensitive to touch while it heals.
It is important to massage the scar with a small amount of water-based hand cream for up to 8 weeks after your procedure. This will help to soften the scar tissue and reduce any sensitivity. For more information, please read the Scar massage leaflet.
Will I need a follow-up appointment?
Most people do not need an appointment following this procedure. You will discuss this with your surgical team.
How soon after surgery can I drive?
You can drive as soon as you feel confident enough to control your car safely and you are not in any discomfort. This is usually about a week after your procedure.
When can I return to my normal activities?
Return to your normal everyday activities as your pain allows. This is often around 1 to 3 weeks after your procedure.
When can I return to work?
Returning to work depends on the type of work you do.
Someone who does heavy manual work may not be able to return for a few weeks.
An office worker may be able to return to light duties a few days after their procedure.
The same applies to sport and the type of sport you play.
What if I have any questions or concerns?
If you have any questions or concerns after your surgery, please contact your consultants secretary. Their contact details will be on your previous hospital appointment letters.
Further information
East Kent Hospitals. Complex regional pain syndrome (CRPS) patient leaflet
East Kent Hospitals: Dupuytren’s disease patient leaflet
[Web sites last accessed 13 March 2026]
What do you think of this leaflet?
We welcome feedback, whether positive or negative, as it helps us to improve our care and services.
If you would like to give us feedback about this leaflet, please fill in our short online survey. Either scan the QR code below, or use the web link. We do not record your personal information, unless you provide contact details and would like to talk to us some more.
If you would rather talk to someone instead of filling in a survey, please call the Patient Voice Team.
Patient Voice Team
Telephone: 01227 868605
Email