Age-related Macular Degeneration (AMD)
Information for patients from Ophthalmology
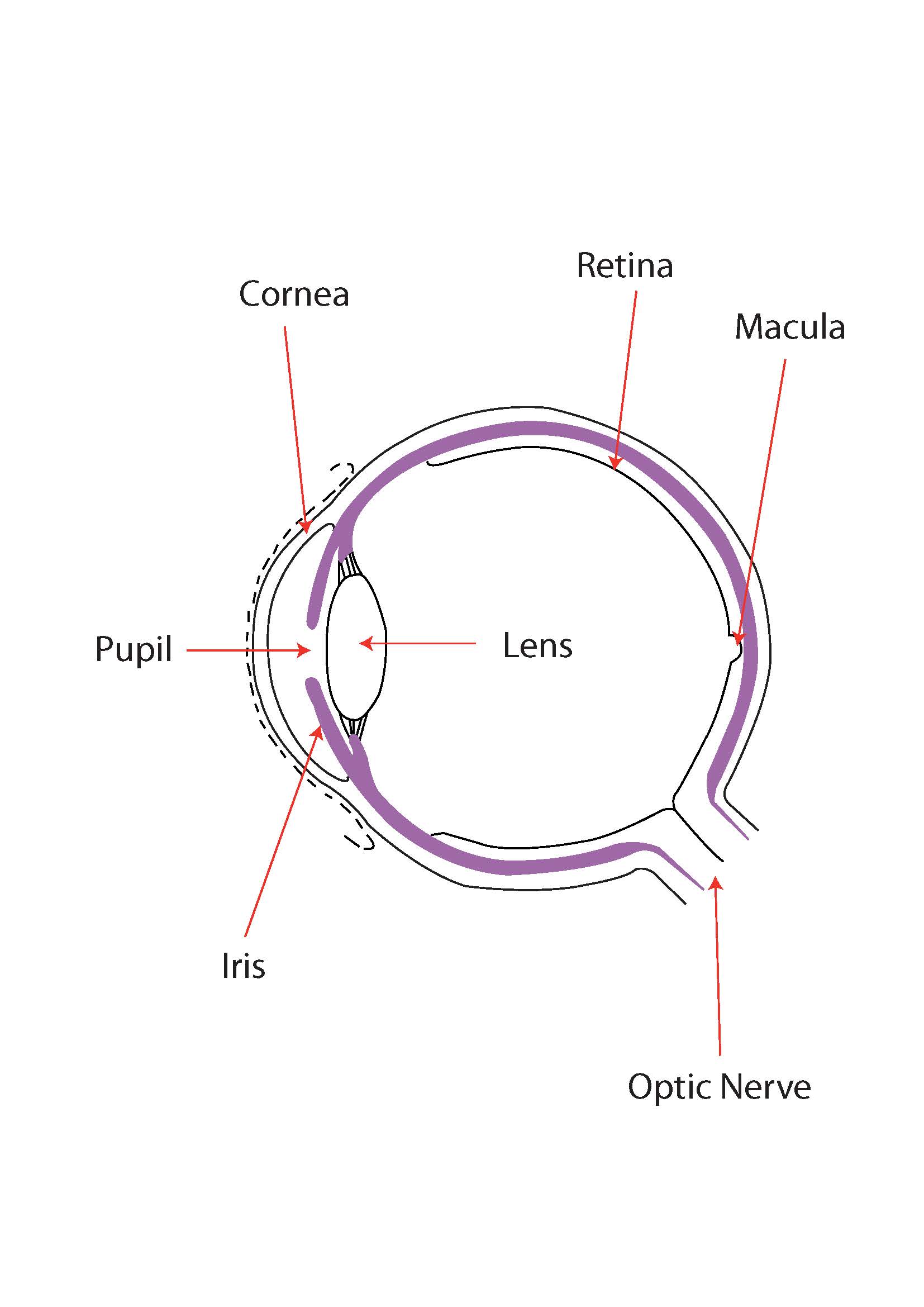
What is Age-related Macular Degeneration (AMD)?
The eye is often compared to a camera, with the retina being the film which captures the image.
The macular is the centre most point of the retina, where the light comes into focus when you are looking at an object. If the macular area is damaged, most people see a blurred spot at the centre of their vision. This is known as macular degeneration. It can cause certain tasks, such as reading, to become more difficult.
What causes Age-related Macular Degeneration?
In most cases there is no known cause. However, it is more common in older people, so it is called Age-related Macular Degeneration.
It is possible for macular degeneration to be hereditary. It can also affect younger people. This is usually known as macular dystrophy.
What are the types of Age-related Macular Degeneration?
There are two types of Age-related Macular Degeneration.
Dry is the most common type. It is caused by slow changes to the macula over many years. In most cases, some useful vision (eyesight) is kept throughout life.
Wet is the less common type. It is usually caused by abnormal blood vessels under the retina. These blood vessels bleed and leak, causing sudden loss of vision.
What is the treatment?
Treatment depends on the type of macular degeneration you have.
Unfortunately, in the case of dry macular degeneration there is no treatment. There is some evidence to suggest that eating fish, fruit, and vegetables (such as broccoli, spinach, and carrots), and not smoking could help. In advanced dry AMD, high doses of vitamins have been shown to reduce the rate of progression. High doses of vitamins are AREDS (Age Related Eye Disease Study) preparations.
Wet AMD can be treated with injections into the eye. These injections reduce the leakage and stop the progression of the disease. To begin with we recommend 3 injections a month. However, based on 4 to 8 weekly assessments, you may need treatment for up to 2 years.
What are the risks to having the injection?
Complications include inflammation and raised pressure in the eye. More rarely you may develop an infection, a retinal detachment, or bleeding.
Any of these complications can result in loss of vision.
What do I do after my injection?
After your injection, we will put lubricating drops in your eye. If your eye feels uncomfortable after your injection, we will give you drops to put in your injected eye for up to 3 days.
You may have some blurred vision, often described as ‘seeing spots floating in the eye’. This can last for up to 2 weeks following your procedure.
You may feel some discomfort in your injected eye. Taking your usual painkillers may help.
If you have increased blurring, pain, or redness in the days after your injection, please contact us.
Ophthalmology Clinic contact details
Monday to Friday 8:30am to 4pm, contact the AMD Co-ordinator at Kent and Canterbury Hospital.
AMD Co-ordinator
Telephone: 01227 783172
If the AMD Co-ordinator is not available, go to your nearest Emergency Department.
Is there any practical help that may help me cope with my condition?
Yes.
Use large print books for reading.
Use angle poise lamps and brighter bulbs, although you may not be able to tolerate bright light. You may find that photochromatic lenses in your glasses help stop some of the glare.
Magnifiers may be useful; ask at your local Low Vision Aid Clinic.
Try looking at objects from the side of your vision, rather than looking directly at them.
Sit closer to the television; this should not adversely affect your vision.
If your consultant considers your vision to be bad enough, they may register you as partially sighted or blind. This may entitle you to additional help. This can include rent rebates, a disabled parking permit, reduced television licence fees, and a free radio / cassette player.
It is important to remember that AMD does not lead to total blindness. However, your central vision will become increasingly difficult to maintain. Your peripheral vision (side vision) should remain less affected.
Useful contacts
Macular Disease Society
Telephone: 01264 350551
EmailKent Association for the Blind (KAB)
Telephone: 01622 691357
Email
What do you think of this leaflet?
We welcome feedback, whether positive or negative, as it helps us to improve our care and services.
If you would like to give us feedback about this leaflet, please fill in our short online survey. Either scan the QR code below, or use the web link. We do not record your personal information, unless you provide contact details and would like to talk to us some more.
If you would rather talk to someone instead of filling in a survey, please call the Patient Voice Team.
Patient Voice Team
Telephone: 01227 868605
Email